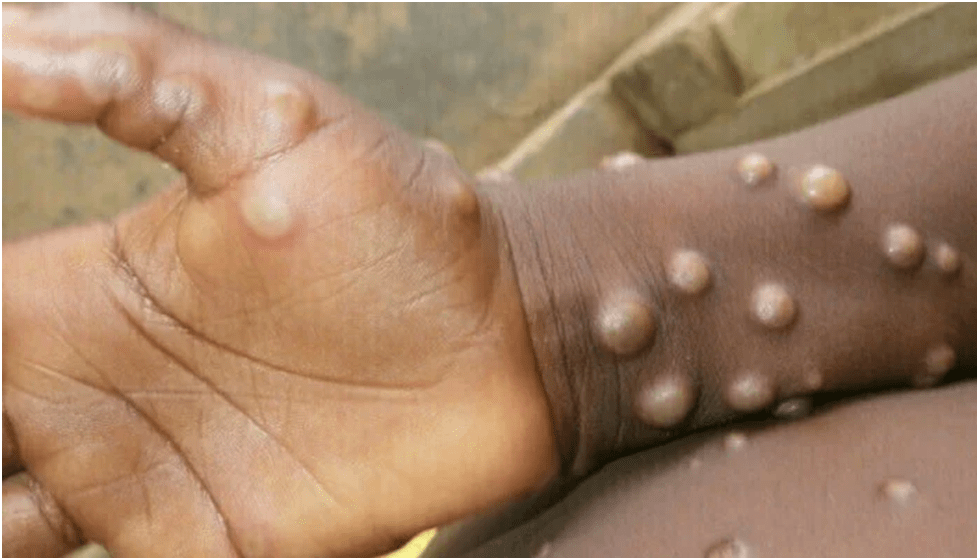
After two years of hearing about the coronavirus, Americans are suddenly aware of another infectious disease: monkeypox.
According to the CDC, there are currently one confirmed case and four suspected cases of the monkeypox virus — a rare disease closely related to smallpox – in the United States.
There are two strains of the virus: one from Central Africa and a less severe variant from West Africa. Recent cases of monkeypox were caused by a virus from West Africa. The confirmed case in the United States is a man from Massachusetts who just visited Canada.
All four suspected cases – one in Florida, one in New York City, and two in Utah – involved men. They have tested positive for the orthopoxvirus family, including smallpox and monkeypox.

Jennifer McQuiston, DVM, deputy director of the CDC’s Division of High Consequence Pathogens and Pathology, stated that individuals with probable cases had recently traveled worldwide; however, specific places were not published due to privacy concerns.
On Monday, local health officials said that a male just returned from a country with incidences of monkeypox has been diagnosed with the virus in Seattle.
According to the World Health Organization, there are currently over 90 confirmed cases and roughly 28 suspected cases of monkeypox in twelve countries.
This outbreak is remarkable because cases have appeared in regions where the virus is rarely seen, including Australia, Canada, the United Kingdom, and other European countries.
In the United States, the CDC anticipates discovering additional monkeypox cases in the following days and weeks.
While monkeypox is a concern, President Joe Biden believes that a quarantine to prevent its spread is probably unnecessary.

“I don’t believe it warrants the same level of concern as COVID-19, and the smallpox vaccination is effective,” he stated at a recent news conference.
Why is monkeypox currently spreading?
According to Aaron Glatt, MD, chair of the Department of Medicine at Mount Sinai South Nassau hospital in New York, the causes underlying the current global pandemic are unknown or have not been made public.
However, while some issues about monkeypox remain unresolved, the virus is not unique.
Monkeypox is endemic in Western and Central Africa, where most cases have been reported since the discovery of the virus. McQuiston told reporters at a recent news conference that many instances of monkeypox have emerged in Nigeria over the past five years, leading to infections in at least nine persons from various parts of the world who had recently returned from the nation.
Human monkeypox cases have already been identified in the United States, including two travelers to Nigeria in 2021. In 2003, 47 confirmed and probable cases were discovered in the United States. According to the CDC, these were directly related to animals imported from Ghana.
Recent global instances of monkeypox were detected in individuals who had not traveled to West Africa or other regions where the virus is prevalent. Infected individuals had gone to Europe and Canada, where cases were detected in late April and early May.
What are the Monkeypox Symptoms?
- The symptoms of monkeypox are comparable to those of smallpox but are less severe. Typically, they occur a week or two after contact with the virus, though they may take longer in rare circumstances.
- Typical initial signs of monkeypox include fever, chills, a headache, and achy muscles.
- In contrast to smallpox and chickenpox, lymph node enlargement is prevalent. (It is important to note that despite their similar-sounding names and descriptions, the chickenpox virus is not linked to the monkeypox virus.)
- After 1 to 3 days of experiencing these symptoms, a rash typically appears on the face, which can subsequently extend to the rest of the body.
- Next, the most prominent symptoms may emerge: flat, circular lesions in various body places that eventually transform into fluid-filled lumps.
- Eventually, these lumps grow crusty and fall off. Even without treatment, recovery typically takes between two and four weeks.
How is monkeypox transmitted?
Primarily, monkeypox is transmitted through close, skin-to-skin contact with individuals who have lesions caused by the virus. You can also contract the virus through respiratory droplets if you are near an infected person with mouth lesions for an extended period.

McQuiston explains, “What we’re talking about here is close touch; it’s not a case where someone passing you in the grocery store is at danger for monkeypox.” According to the CDC, to limit the spread of the virus, it is best to confine infected individuals and monitor their close connections. To prevent the spread of monkeypox, some health experts propose a “ring vaccination” method, which involves vaccinating the close contacts of an infected individual.
Exist Vaccines Against Monkeypox?
According to the CDC, the effectiveness of the smallpox vaccine against the monkeypox virus is at least 85 percent.
Currently, the United States has one antiviral and two FDA-approved vaccinations to prevent smallpox.
One, a more recent vaccination called Jynneos, is also approved to combat monkeypox. If a person is at high risk for smallpox or monkeypox and is 18 years or older, they can receive the two-dose vaccine.
According to McQuiston, the United States possesses approximately 1,000 doses of the Jynneos vaccine and has requested more from the National Stockpile for “high-risk contacts of some of the early patients” according to McQuiston.
The United States also owns more than 100 million doses of ACAM2000, an older smallpox vaccine. However, health officials are cautious about distributing it to the general public due to its severe adverse effects.
According to John Brooks, MD, a medical epidemiologist with the CDC’s Division of HIV/AIDS Prevention, these side effects can be particularly severe for immunocompromised or eczema-afflicted individuals.
Currently, most people who receive smallpox immunizations have been exposed to monkeypox or who “have a compelling cause to get the vaccine,” according to Glatt.
At this time, you would not provide this to the broader populace.
How Are Cases of Monkeypox Confirmed?
Testing occurs in two phases.
Initially, patient test samples are forwarded to state laboratories for orthodox testing.
If tests are positive, samples are sent to the CDC for testing for monkeypox.
Do I Need a Special Kind of Doctor for Treatment of Monkeypox?
If you believe you have contracted monkeypox, you can consult your local physician. Brooks states, “This is a disease that can be managed or detected in a general physician’s office using ordinary standard precautions, so we’re encouraging front-line doctors to be alert.”
According to him, health care personnel can protect themselves from monkeypox by donning gloves, an N95 respirator, a face mask, and possibly a protective gown.
Who Is the Most Vulnerable to Monkeypox?
Anyone can become sick and transmit monkeypox following close contact with the virus. However, the majority of current cases have been detected among gay and bisexual populations and other men who have sex with other men.
Even though monkeypox is not classed as an STD, the virus can be transmitted “via sexual and intimate contact and through personal contact in sharing bedding and clothing,” according to Brooks.
He notes that monkeypox can also be confused for certain STDs, mainly when vaginal and anus lesions are present. “One thing I’d want to mention about the condition is that the lesions and rashes have been abnormal compared to expected,” Brooks says.
A physician first suspected that a patient had severe herpes in one instance.
He advises that anyone who develops an inexplicable rash should consult a physician immediately to rule out monkeypox and other sexually transmitted diseases.
How Threatening Is the Monkeypox Virus?
The current outbreak of monkeypox in the United States and Europe has produced minimal symptoms. However, the virus can cause severe health issues, especially in immunocompromised individuals and those with skin diseases like eczema.
Lesions that form in particular areas of the body might be very dangerous. According to McQuiston, lesions in the eye may result in visual loss.
And if the virus causes your lymph nodes to grow, breathing may become difficult.
“Fortunately, we have antivirals available for treatment, which can be administered to individuals at a higher risk for severe disease or who already have severe disease,” explains Brooks.
How is monkeypox dissimilar to COVID-19?
According to the CDC, the viruses are distinct in two significant aspects.
COVID-19 is highly contagious, primarily through the liquid droplets produced when infected people cough, sneeze, or speak.
On the other hand, monkeypox is primarily transmitted through bodily fluids, viral sores, and respiratory droplets of infected individuals with lesions in their mouths and throats.
Secondly, the COVID-19 virus targets the upper respiratory tract, causing sore throat and coughing instead of the flu-like symptoms of monkeypox.
“Early on in COVID-19, we didn’t have much knowledge, and as we learned more, the situation evolved,” McQuiston explains. Many decades of research have taught us about monkeypox, and respiratory dissemination is not the primary concern.
Could Animals Catch Monkeypox?

Given that monkeypox is a zoonotic virus, which means it originates in animals, it can spread to humans and other species during a “spillover event.”
However, according to McQuiston, cats, dogs, and other pets are not thought to be at significant risk of infection.
“During the 2003 outbreak of monkeypox, we conducted extensive testing on various animal species, and we did not observe any spread to household pets,” she explains.
However, I believe this is a subject we will continue to monitor closely.
Would the effectiveness of a smallpox vaccine against monkeypox diminish with time?
Many elderly persons have presumably already had the smallpox vaccine. Glatt says that protection diminishes over time while there is some advantage.
Even these individuals, if exposed, would likely require a second dose of the smallpox vaccine.
Could Monkeypox Become the Next Global Epidemic?
According to Glatt, a pandemic of monkeypox is exceedingly unlikely.
“The transmission channels are distinct from COVID-19,” he explains. “Long-term, close human-to-human interaction is required, but it is not widespread. COVID-19 is highly prevalent among humans.
